NHS limiting access to essential obesity services across England, British Medical Journal reveals
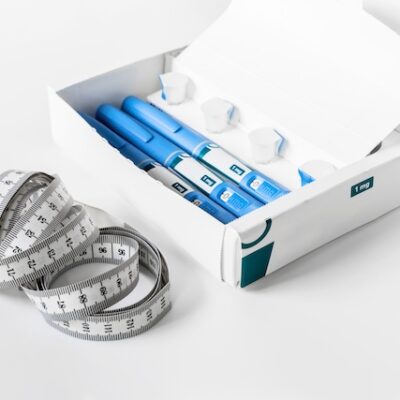
The National Health Service (NHS) is restricting access to crucial obesity services across England, leaving individuals in nearly half of the country without the ability to seek appointments with specialist teams for necessary support and treatments, including weight-loss injections.
This concerning situation was uncovered through an investigation by the British Medical Journal (BMJ), which mirrors the findings of a recent report by the Future Health research agency. The agency’s report highlighted that many of England’s Integrated Care Boards (ICBs) have failed to establish detailed strategies to address obesity and provide treatment, despite the condition costing the United Kingdom an estimated £98 billion annually in healthcare expenses, lost productivity, and other associated costs.
Richard Sloggett, the report’s author and a former special adviser in the Department of Health and Social Care, described these new revelations as evidence of the NHS “rationing” obesity treatment. He emphasised, “These findings back up our Future Health research showing that many ICBs do not currently see obesity as a priority. In certain parts of the country, there is no access to tier 3 and tier 4 services at all. This rationing is leading to a postcode lottery of care. Given the scale of the obesity challenge facing the country and the wider health and economic costs and impacts associated with it, there is an urgent need for the government and the NHS to commit new action. This should start with a clear timeline for reviewing NHS obesity services and ensuring there is a minimum service specification agreed and in place in each ICB.”
A spokesperson for NHS England responded to the BMJ’s investigation by stating that the NHS was “working with the Department of Health to support improvements in the obesity pathway.” However, experts argue that more decisive action is needed.
The BMJ’s investigation also revealed that budget cuts have disproportionately impacted local services focused on obesity care. Individuals living with obesity are often viewed as less deserving of care compared to those with other health conditions, exacerbating the situation. This reality has led to what one expert describes as a “postcode lottery of care,” where access to obesity services varies significantly depending on geographical location.
Data collected through freedom of information requests sent to all 42 of England’s ICBs showed that patients in one in six local healthcare areas were unable to access bariatric surgery, a treatment considered one of the most clinically effective interventions for obesity.
Dr Nicola Heslehurst, a professor of maternal and child nutrition at Newcastle University and chair of the UK Association for the Study of Obesity, voiced her concerns about the current state of weight management services. She told the BMJ, “Current weight management services do not in any way meet the need,” and warned that “radical” action was necessary to combat the rising prevalence of obesity, the associated care costs, and health inequalities. She also stressed the impact on future generations, cautioning that without intervention, children may be “set up for a life course of poor health.”
Obesity imposes a significant financial burden on the NHS in England, costing an estimated £6.5 billion each year. It is also recognised as the second leading cause of cancer after smoking, highlighting the urgency for a comprehensive and effective response.
ICBs receive funding from NHS England to deliver healthcare services for their local communities. However, recent budget cuts have placed immense financial pressure on these boards. In many cases, when resources are limited, services perceived as lower priority are denied funding, with obesity care frequently being the first to face budget reductions.
The BMJ’s investigation found that just over half (24) of England’s 42 ICBs commissioned the full spectrum of adult weight loss services and were open to new referrals. These services range from localised diet and lifestyle classes to more advanced interventions, such as semaglutide weight-loss injections (marketed as Wegovy) and gastric bypass surgery.
However, over a third of ICBs reported imposing restrictions on tier three obesity services, which involve multidisciplinary teams capable of prescribing weight-loss medications. Among these ICBs, six had closed their services to new patients, seven provided services only to certain parts of their catchment area, and four lacked any tier three services altogether.
Tier four services, which include more intensive weight-management interventions like gastric bypass surgery, are also severely restricted. The investigation found that seven ICBs do not offer any bariatric surgery, further highlighting the disparities in access to care across different regions of England.
John Wilding, a professor of medicine at the University of Liverpool, criticised the lack of prioritisation for obesity services, stating, “Obesity services are not deemed a priority.” He also pointed out a prevailing bias within the healthcare system, noting, “I think there is an unconscious bias which says: ‘This is mostly their fault, so they should just get on with it, go on a diet and lose weight.’ But we know from genetics and other factors that it’s much more complicated than that.”
These findings underscore an urgent need for a comprehensive review of NHS obesity services and the establishment of a uniform standard of care across all ICBs. The current restrictions on access to essential obesity treatment services not only create health inequalities but also contribute to escalating healthcare costs and long-term negative health outcomes. Without significant changes in policy and practice, the NHS faces an ongoing struggle to address the obesity crisis effectively.